The end of TB
Syllabus Covered:
GS Paper II - Health & Social Justice
GS Paper III - Science & Tech
Although many believed in the 1980s that tuberculosis (TB) was on the path to elimination, it made a strong comeback due to multiple factors, especially in the United States — re-emerged with more complexity in the late 20th century due to scientific, social, and political neglect.
Historical Timeline & Early Successes
- Mid-20th century: TB cases had been sharply
declining in the U.S. This success was attributed to:
- Better urban sanitation.
- Development and use of antibiotics like streptomycin.
- Widespread vaccination and public health campaigns.
- Improved housing and nutrition.
- By the 1980s, TB incidence had dropped so low that many believed its elimination was inevitable. TB was no longer seen as a major public health threat in developed countries.
Reversal of Gains: The Comeback of TB (Late 1980s–1990s)
Despite early optimism, the 1980s and 1990s saw a shocking resurgence of TB in the U.S. due to the following key reasons:
HIV/AIDS Epidemic:
- HIV weakens the immune system, making people highly susceptible to TB infection.
- Co-infection became common, particularly in urban centers.
Funding Cuts:
- In the early 1980s, the U.S. government cut funding for TB control
programs, leading to:
- Neglect in surveillance systems.
- Reduced investment in public health infrastructure.
- Collapse of once-strong tuberculosis clinics and support mechanisms.
Immigration & Urban Vulnerability:
- S. immigration policy changes in the 1960s allowed more people from TB-endemic countries (Africa, Asia, Latin America) to settle.
- Many of these immigrants had latent TB infections, which could later activate, especially under poor living conditions.
Emergence of Drug-Resistant TB:
- Misuse and incomplete antibiotic treatment led to strains resistant to first-line TB drugs.
- These strains were harder and costlier to treat and more lethal.
Poverty, Overcrowding & Prisons:
- TB outbreaks surged in:
- Homeless shelters.
- Prisons.
- Crowded urban housing.
Between 1985 and 1992, TB cases in the U.S. increased by 20%, reversing decades of progress.
Global Dimensions & WHO Emergency Declaration
- The resurgence wasn’t limited to the U.S.
- Globally, TB was still killing millions, especially in sub-Saharan Africa, South Asia, and parts of Eastern Europe.
- The WHO declared TB a global health emergency in 1993.
- This was due to increasing drug resistance and its synergy with HIV in developing countries.
Scientific and Medical Realities
- Latent TB: Mycobacterium tuberculosis can lie dormant in the body for years, reactivating when immunity drops.
- TB requires long, uninterrupted treatment (6–9 months). Many patients discontinue midway, risking resistance.
- Treating multi-drug-resistant TB (MDR-TB) is costly, time-consuming, and comes with severe side effects.
What Went Wrong?
- The main error was overconfidence.
- By the 1980s, TB was so rare in developed countries that it was de-prioritized in policy and funding.
- Public health experts and doctors warned about possible resurgence, but their voices were largely ignored.
- The system failed to:
- Maintain early detection
- Adapt to new risk groups (HIV patients, immigrants).
- Monitor drug resistance trends in time.
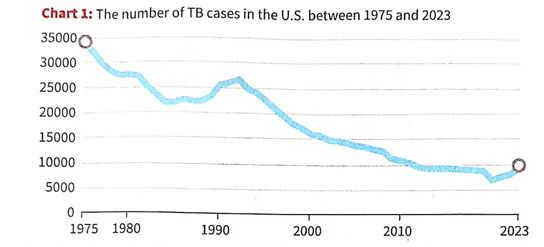
Data and Charts (from the article)
- Charts in the article show:
- A steep drop in TB cases till the early 1980s.
- A spike in the 1990s due to the factors above.
- Correlation between HIV rates and TB incidence.
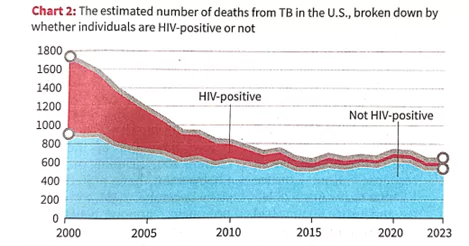
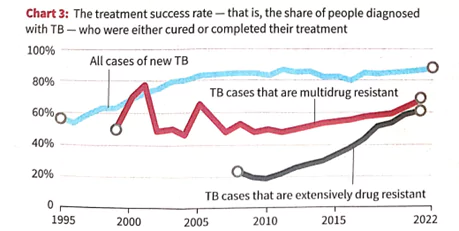
Lessons for India and the World
- TB is not just a biological disease; it's deeply rooted in poverty, neglect, and systemic failures.
- Elimination requires:
- Consistent funding, even when case numbers are low.
- Community-level surveillance.
- Global cooperation—as migration and travel affect all countries.
- Addressing co-morbidities like HIV, malnutrition, and diabetes.
- Investment in R&D for shorter, safer treatment regimens and better vaccines.
Prelims Questions:
- Which of the following factors contributed to the resurgence of
Tuberculosis (TB) in the United States during the late 1980s and early
1990s?
- The spread of HIV/AIDS
- Emergence of drug-resistant TB strains
- Increased immigration from TB-endemic countries
- Enhanced diagnostic facilities leading to over-reporting
- 1, 2 and 3 only
- 2 and 4 only
- 1, 3 and 4 only
- 1, 2, 3 and 4
- Consider the following statements regarding Tuberculosis (TB):
- TB bacteria can remain dormant in the human body and reactivate later.
- The World Health Organization declared TB a global health emergency in the year 1993.
- TB treatment generally requires a short course of antibiotics lasting about 10-15 days.
- 1 and 2 only
- 2 and 3 only
- 1 and 3 only
- 1, 2, and 3
- The declaration of TB as a “global health
emergency” by WHO was primarily triggered by:
- The development of a highly contagious airborne variant of TB
- Increasing cases of TB among children worldwide
- The emergence of multidrug-resistant TB strains and HIV-TB co-infection
- A pandemic-like global spread of TB within a single year
Select the correct answer using the code below
Answer: A
Explanation:
TB's resurgence in the U.S. was due to HIV/AIDS, drug resistance, and immigration from TB-endemic countries. Over-reporting due to enhanced diagnostics was not a reason.
Which of the above statements is/are correct?
Answer: A
Explanation:
Statement 3 is incorrect — TB treatment typically requires 6–9 months, not 10–15 days.
Answer: C
Explanation: The WHO declared TB a global emergency in 1993 primarily due to the dual burden of HIV-TB co-infection and rising drug resistance.
Mains Question:
- “Despite advances in treatment and diagnostics, TB remains a major global health challenge.” In light of this, discuss the factors behind TB resurgence and measures needed for effective TB control and elimination.